 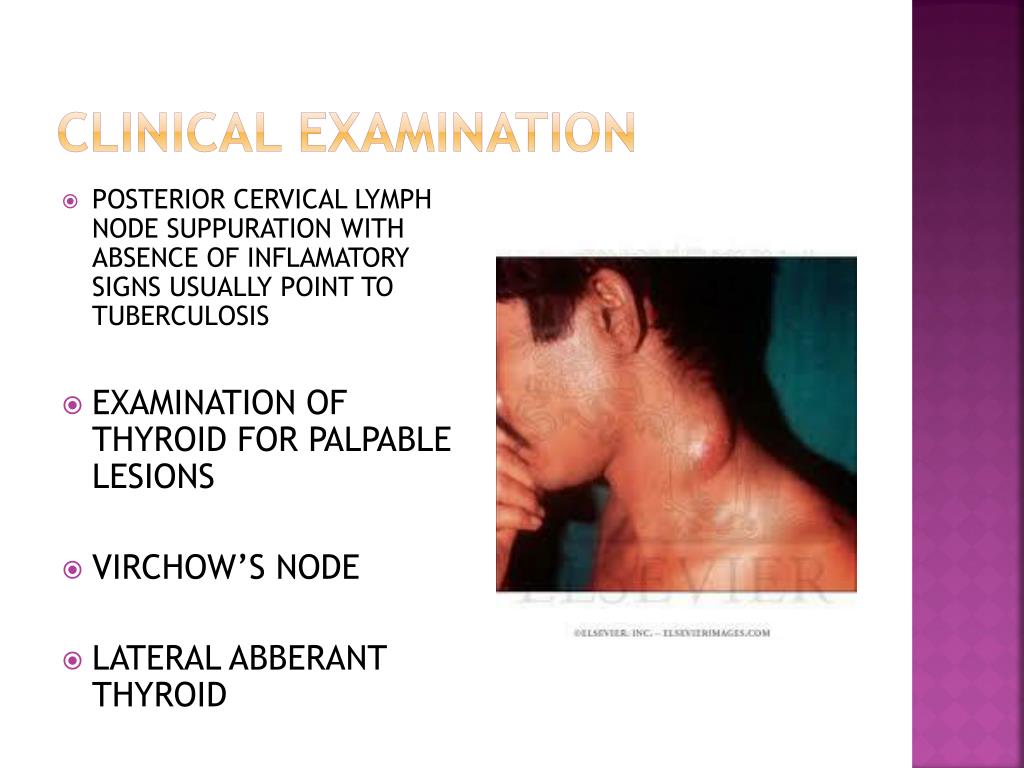 
Based on these promising results, we hypothesize that T1 and T2 mapping can be utilized to differentiate between metastatic lymph nodes and reactive lymph node hyperplasia in HNSCC. Recent studies have confirmed the potential clinical utility of T1 and T2 mapping techniques in distinguishing between benign and metastatic lymph nodes in mesenteric lymph nodes for rectal cancer and in retropharyngeal lymph nodes for nasopharyngeal cancer. T1 and T2 mapping techniques have been successfully applied in various types of cancer, including the differential diagnosis of benign and malignant lesions and the prediction of pathologic features of cancer. It allows for visualizing quantitative T1 and T2 relaxation times, providing more reproducible data reflecting intrinsic biological tissue characteristics and microstructural differences within lesions. Quantitative mapping of longitudinal relaxation time (T1) and transverse relaxation time (T2), initially introduced in studies involving the myocardium, musculoskeletal system, and central nervous system, has increasingly extended to the investigation of various tumors. 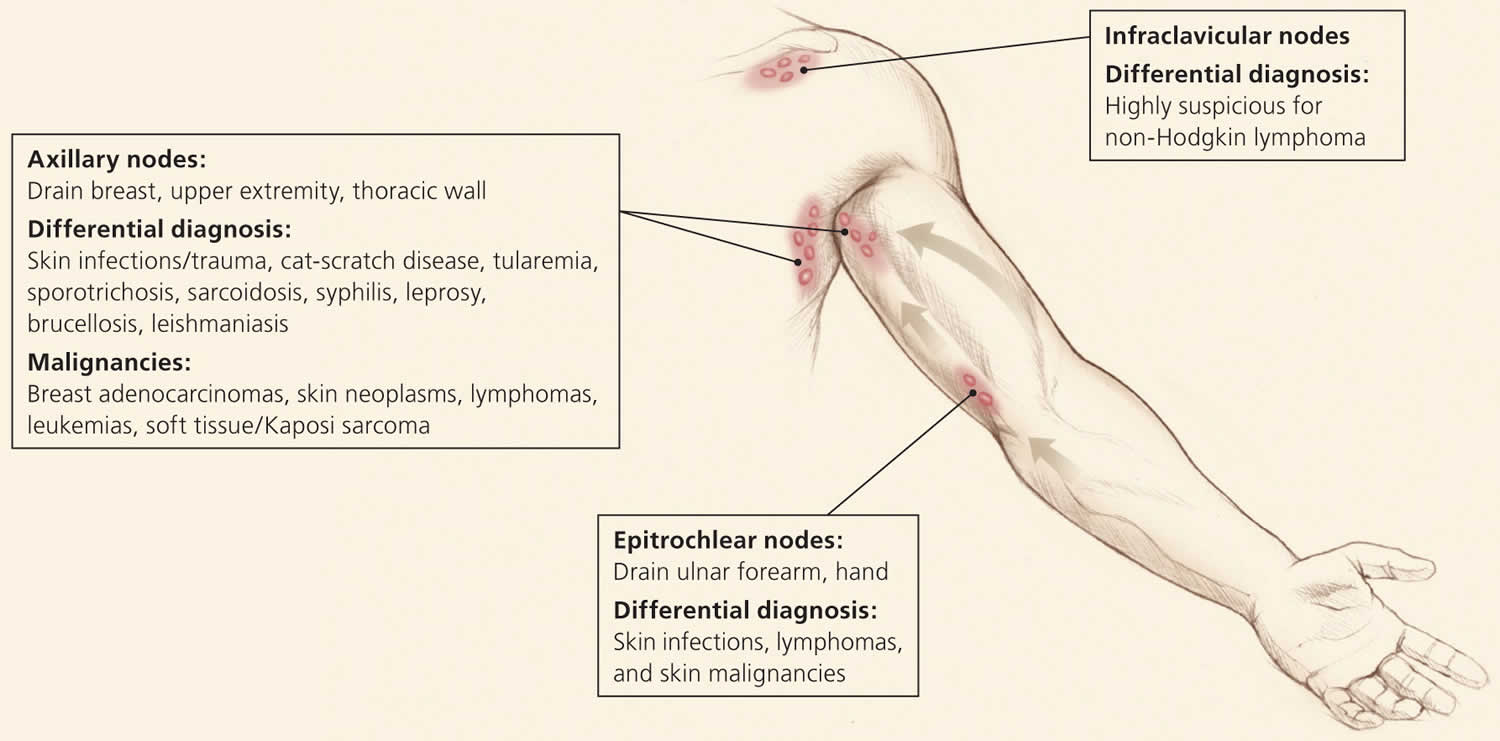
Therefore, it is necessary to identify a more objective and accurate quantitative method for distinguishing between metastatic and non-metastatic lymph nodes. Malignant and benign nodes have been reported to exhibit significant overlap in apparent diffusion coefficient (ADC) values, which can be influenced by various imaging conditions. Although DWI is an essential functional imaging modality widely used to distinguish between benign and malignant lesions, it has been controversial in differentiating lymph node status in HNSCC. Diffusion-weighted imaging (DWI), a non-invasive imaging technique that characterizes tissues based on the restricted diffusion of water molecules, is a simple sequence included in routine head and neck MRI. However, defining lymph node metastasis on MRI without apparent signs of extranodal extension (ENE) or intranodal necrosis is often challenging due to the less reliable size and morphology criteria. MRI has been proven to be a valuable tool for evaluating nodal staging in HNSCC. Currently, the gold standard for diagnosing cervical lymph node metastasis remains postoperative pathological examination. The management of the neck is complicated in HNSCC since it involves different combinations of treatment strategies, and accurate preoperative evaluation of cervical lymph node metastasis still remains challenging. The application of T1 and T2 mapping is feasible in differentiating metastatic from non-metastatic lymph nodes in HNSCC and can improve diagnostic efficacy compared to DWI.Ĭervical lymph node metastasis in head and neck squamous cell carcinoma (HNSCC) is a crucial prognostic factor, significantly reducing disease-free survival and worsening overall prognosis, and it necessitates more aggressive treatment and follow-up. Combining T2, T1 SD, ADC, and lymph node size achieved an AUC of 0.929 (0.875–0.983), which did not significantly enhance diagnostic performance over using T2 alone ( p = 0.089). Conversely, metastatic lymph nodes exhibited significantly higher apparent diffusion coefficient (ADC) and standard deviation of T1 values (T1 SD) ( p < 0.001). Mean T2 values for metastatic lymph nodes were significantly lower than those for benign lymph nodes ( p < 0.001). We examined a total of 122 lymph nodes, 45 (36.9%) of which were metastatic proven by pathology. Receiver operating characteristic curves and the DeLong test were employed to determine the most effective diagnostic methodology. Quantitative measurements derived from preoperative T1 and T2 mapping and DWI of metastatic and non-metastatic lymph nodes were compared using independent samples t-test or Mann–Whitney U test. Methodsīetween July 2017 and November 2019, 46 HNSCC patients underwent neck MRI inclusive of T1 and T2 mapping and DWI. This study seeks to assess the utility of T1 and T2 mapping in distinguishing metastatic lymph nodes from reactive lymphadenopathy in patients with head and neck squamous cell carcinoma (HNSCC), using diffusion-weighted imaging (DWI) as a comparison. 
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
